Patients first!
#NothingAboutUsWithoutUs
It might seem obvious that patient needs should have highest priority in healthcare. But we believe that this isn’t always the case.
Healthcare has become a huge and complex industry with many different stakeholders, each with their own aims. These objectives are not necessarily identical with those needing care and treatment from the system.
The market system creates incentives and constraints, which may not coincide with the greatest benefit of patients.
Regulation and supervision exist to protect patients from possible damage and ensure best care, but these cannot fully resolve the fundamentally divergent interests between different stakeholders.

In personal care treatments are usually chosen and administered on the decision of healthcare professionals. We believe that particularly in chronic disorders, such as rheumatic and musculoskeletal diseases, patients living 24/7 for many years with their conditions have acquired much knowledge about disease management, and the effects of treatments and care.
This knowledge doesn’t find its way into care plans and is not always solicited. If patient knowledge were to be used in scientific research, it would help ensure that the right questions are being asked, and research efforts would be relevant to patients’ needs.
This is the starting point for RheumaCura: to include and integrate patient wisdom into research and the development of better healthcare.
Patient-centred research
Patients are a source of information and understanding that are often overlooked in medicine. The concept of engaging patients in healthcare is neither new nor complex, however it has not yet been adopted widely in Switzerland.
Patient-centred research is part of an integrated concept embracing collaborative efforts between scientists with different specialist skills, clinicians and other health care workers, patients and their families and close others.
Such collaboration should make research more relevant to patients’ needs and thus ultimately lead to better care, treatments and prevention.

“Nothing About Us Without Us”
Patient-centred research emphasises that research being carried out ‘with’ or ‘by’ members of the public and patients, rather than ‘to’, ‘about’ or ‘for’ them. It covers not only the involvement but also explicitly recognises that medical research should always be centred around the patient, and not driven by profit motives or professional ambitions.
The continuum of patient engagement
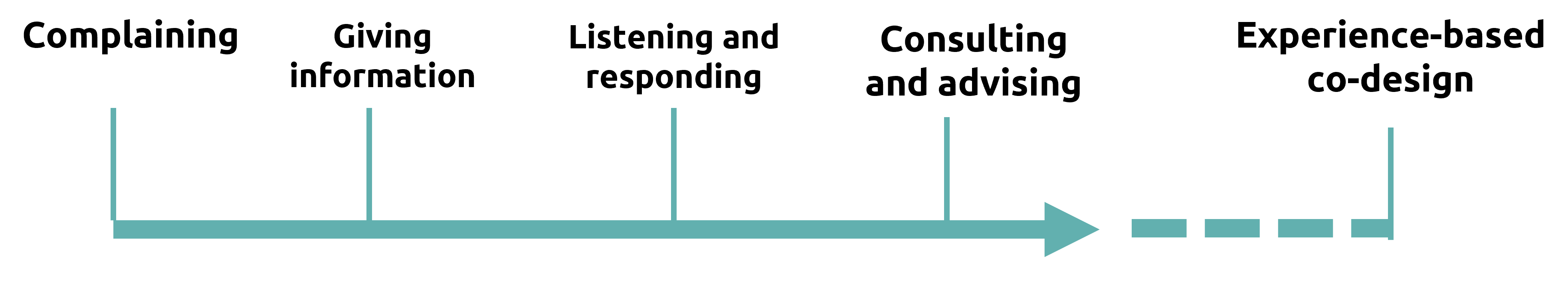
Patient engagement begins with structures to enable feedbacks and complaints about services. They may be asked to participate in surveys or focus groups. Experience has shown that resulting recommendations seldom lead to change.
The most effective level of engagement is when patients can actively contribute with their knowledge and experience through co-construction in research projects, and patients are involved in the whole research cycle from ensuring that the right questions are asked to the introduction of new treatments and their evaluation.
RheumaCura aims to involve patients at the highest levels of engagement.
Understanding and Contributing
Patients want to be listened to and bring their needs and ideas into healthcare to improve it. We believe that they have much to contribute.
We understand our work as a form of citizens’ science because research supported by RheumaCura will be conducted with patient participation, sometimes called "user involvement".
The two dimensions of the relationship between citizens and science:
- science should be responsive to citizens' concerns and needs;
- citizens themselves can produce reliable scientific knowledge.

Patient-centred research addresses both these aspects. Here are some of the questions in a research project that patients’ knowledge and experience can help to answer:
-
Are the right questions being asked and the factors of concern for patients really being addressed in the research?
-
What factors must be considered when designing and preparing a research project, so that it is relevant to patients?
-
Who are the most suitable patient participants to recruit for a project, and where can they be found?
-
How to collect, interpret and analyse the data as “real-world evidence” meaning the knowledge that is relevant to those affected by disease?
-
How to ensure that new knowledge is made known and safely integrated into the health care system and clinical practice to help patients?
-
How to monitor and evaluate the “real-world” results of the research and learn for future activities?
These questions show that patients can be involved along the whole research chain from developing the research questions to supporting efforts to get the results known and available to those needing them.
Equally patients want to learn, both from other patients and from healthcare professionals. This can help them to manage their own conditions, and contribute to improving health care.
It is by sharing knowledge, understanding each other, and contributing to collaboration, that healthcare improvements, innovation and new ideas are created.
What Matters To You?
Think about the difference between "What Matters To You?" and "What is the matter with you?"
The first question is compassionate and focused on the needs of the patient. The second question is analytical and implies that something is not ok about the person. This second question is important and often asked in healthcare, but it can be demeaning.
At RheumaCura we believe that the first question is equally important, it is empowering and not asked often enough.
“What Matters to You?” was inspired by an article written by two patient advocates Michael Barry and Susan Edgman-Levitan, called Shared Decision-Making: The Pinnacle of Patient-Centered Care, which was published in the renowned New England Journal of Medicine in 2012. Both authors have dedicated their careers to strengthening the patient's voice in healthcare. Michael J. Barry is a physician researcher and Susan Edgman-Levitan is a patient advocate affected by rheumatic disease and founding President of the Picker Institute: an international centre of innovation to improve patient-centred healthcare.

“What Matters to You?” (WMTY) is now an international movement which is celebrated on 9th June. It helps healthcarers to understand what is “most important” to patients by following the principle, "Ask, listen, do" what matters. This shifts the power to the person who knows best about the help or support they need, whether it be a person with a medical issue or the clinicians or staff providing care. WMTY conversations help healthcare teams understand what is most important to patients and leads to better care partnerships and improved patient experience.
The WMTY movement has spread to over 49 countries from the USA and UK to Australia, Brasil, Denmark and Estonia and including Switzerland through the Federation of Vaudois hospitals. WMTY has been integrated into workflows in hospitals, primary care, behavioral health, substance use treatment programmes and community based social service organizations.
What about patient-centred research into rheumatic and musculoskeletal diseases?
The "What Matters To You?" approach changes the paradigm of how patients are treated in healthcare and in research. You can read more about how we want to approach research here.

